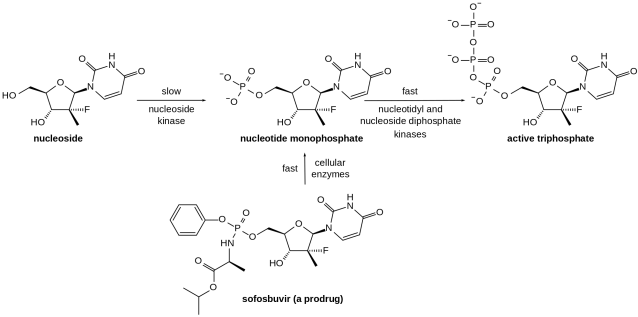
Sofosbuvir (brand name Sovaldi) is a nucleotide analog used in combination with other drugs for the treatment of hepatitis C virus (HCV) infection.
An analysis of a new drug’s journey to market, published this week in the BMJ, shines a light on financial practices that see some major pharmaceutical companies relying on a cycle of acquisitions, profits from high prices, and shareholder-driven manoeuvres that threatens access to medicines for current and future patients.
New research on the financial practices surrounding a ‘wonder drug’ with a more than 90% cure rate for hepatitis C – a blood-borne infection that damages the liver over many years – shows how this medical breakthrough, developed with the help of public funding, was acquired by a major pharmaceutical company following a late-stage bidding war.
The research shows how that company more than doubled the drug’s price over original pricing estimates, calculating “how much health systems could bear” according to researchers, and channelled billions of dollars in profits into buying its own shares rather than funding further research.
In this way, the company, Gilead Sciences, passed significant rewards on to shareholders while charging public health services in the US up to $86k per patient, and NHS England almost £35k per patient, for a three month course of the drug.
The high prices have contributed to a rationing effect: many public systems across the US and Europe treat only the sickest patients with the new drug, despite its extraordinary cure rate, and the fact that earlier treatment of an infectious disease gives it less opportunity to spread.
Gilead’s strategy of acquisitions and buybacks is an example of an industry-wide pattern, say the researchers. Many big pharmaceutical companies now rely on innovation emerging from public institutes, universities, and venture-capital supported start-ups – acquiring the most promising drug compounds once there is a level of “certainty”, rather than investing in their own internal research and development.
The researchers, from Cambridge University’s Department of Sociology, say this effectively leaves the public “paying twice”: firstly for the initial research, and then for patent-protected high priced medications. A summary of their research has been commissioned by the British Medical Journal (BMJ) and was published this week.
“Large pharmaceutical companies rarely take a drug from early stage research all the way to patients. They often operate as regulatory and acquisition specialists, returning most of the subsequent profits to shareholders and keeping some to make further acquisitions,” said lead researcher Victor Roy, a Cambridge Gates Scholar.
The study’s senior author, Prof Lawrence King, said: “Drug research involves trial and error, and can take years to bear fruit – too long for companies that need to show the promise of annual growth to investors, so acquisitions are often the best way to generate this growth.”
There are an estimated 150 million people worldwide chronically infected with hepatitis C. It disproportionately affects vulnerable groups such as drug users and HIV sufferers, and can ultimately lead to liver failure through cirrhosis if left untreated.
Roy and King’s article tells the story of the curative drug Sofosbuvir. The compound was developed by a start-up that emerged from an Emory-based laboratory that received funding from the US National Institutes of Health and the US Veterans Administration.
The start-up, Pharmasset, eventually raised private funding to develop sofosbuvir. When Phase II trials proved more promising than Gilead’s in-house hepatitis C prospects, it acquired Pharmasset for $11bn following a bidding war – the final weeks of which saw Pharmasset’s valuation rocket by nearly 40%.
“The cost of this late stage arms race for revenues has become part of the industry justification for high drug prices,” write Roy and King.
Once Sofosbuvir was market-ready in 2013, Gilead set a price of $84k. A US Senate investigation later revealed that Pharmasset had initially considered a price of $36k.
By the first quarter of 2016, Gilead had accumulated over $35bn in revenue from hepatitis C medicines in a little over two years – nearly 40 times Gilead and Pharmasset’s combined reported costs for developing the medicines.
Last year, Gilead announced that a lion’s share of those profits – some $27bn – will go towards ‘share buybacks’: purchasing its own shares to increase the value of the remaining ones for shareholders. By contrast, between 2013 and 2015 Gilead increased research investment by $0.9bn to $3bn total.
“Share buybacks are a financial manoeuvre that emerged during the early 1980s due to a change in rules for corporations by the Reagan administration. The financial community now expects companies to reward shareholders with buybacks, but directing profit into buybacks can mean cannibalising innovation,” said Roy.
A further example they cite is that of Merck, who spent $8.4bn in 2014 to acquire a drug developer specialising in staph infections. The next year they closed the developer’s early stage research unit, laying off 120 staff. Three weeks after that, Merck announced an extra $10bn in share buybacks.
In the BMJ article, the researchers set out a number of suggestions to counter the consequences of the current financial model. These include giving health systems greater bargaining power to negotiate deals for breakthrough treatments, and limiting share buybacks.
Roy and King also highlight a possible future model that uses a mix of grants and major milestone prizes to “push” and “pull” promising therapies into wider application, and, crucially, uncouples drug prices from supposed development costs, including those added by shareholder expectations. They write that this approach may be attempted for areas of major public health concern.
“The treatments for Hepatitis C may portend a future of expensive therapies for Alzheimer’s to many cancers to HIV/AIDS. Health systems and patients could face growing financial challenges,” said King.
“We need to recognise what current business models around drug development might mean for this future.”
Source: University of Cambridge
Categories: Breaking News, Leadership in Health, Leadership in Medicine















