A molecule best known for its involvement in pain perception also plays an important role in regulating body weight, according to new studies in mice by scientists at the Howard Hughes Medical Institute’s Janelia Research Campus. The molecule, called Nav1.7, enables some neurons to efficiently integrate information they receive over time. When weight-regulating neurons lose this ability, mice become either over- or underweight.
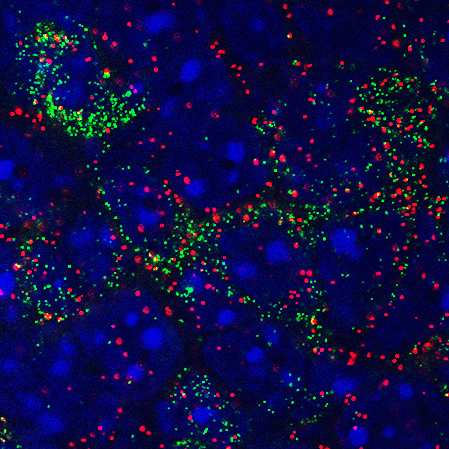
The image shows coexpression of Agrp (green) and the sodium channel Nav1.7 (red) in neurons in the hypothalamus. Credit: Sternson Lab, HHMI/Janelia Research Campus
Janelia group leader Scott Sternson, who led the research, says Nav1.7 equips cells to remember input they have received, so that they can integrate it with information that arrives later. That’s important for regulating appetite, a process that unfolds over minutes to hours. Sternson and his colleagues reported in the June 16, 2016, issue of the journal Cell that Nav1.7 makes cells “near-perfect integrators” of incoming information.
The circuits in the brain that manage the body’s energy needs integrate information from many sources. The weight-regulating neurons Sternson and his colleagues study are controlled in part by signals they receive from hormones, such as ghrelin and leptin. “These neurons have the bizarre property of integrating their inputs over very long timescales,” Sternson says. Whereas most neurons must integrate multiple signals that arrive all at once, appetite-regulating neurons must remember and integrate the signals they receive over about half a second, firing only if enough signals arrive during that time. That’s more than 10 times longer than the period over which most neurons integrate input, Sternson says. The ability of these neurons to efficiently track their inputs over time is related to the tendency for our bodies keep track of calorie intake and output.
Sternson and Tiago Branco, a neuroscientist collaborating with Sternson through Janelia’s Visiting Scientist Program, wanted to understand how certain cells integrate information over prolonged periods of time. To look for clues, they experimented with AGRP neurons, which are cells located in the brain’s hypothalamus that produce signals that drive animals to eat. Sternson and Branco, who is now at the MRC Laboratory for Molecular Biology in Cambridge, England, found that if they chemically switched off membrane channels that regulate the passage of sodium ions into the cell, AGRP neurons failed to integrate incoming signals.
With their attention focused on sodium channels, they realized that one such channel — Nav1.7 — was prevalent in AGRP cells, even though it had not previously been reported to be present in this part of the brain. The channel is essential for the perception of pain, but Sternson and his team found that it was widespread in the hypothalamus — not only in AGRP neurons, but in many cell types associated with hormonally-regulated processes, including other body weight-regulating neurons.
When the scientists blocked the Nav1.7 channel in several of these cell types, the neurons’ ability to integrate incoming signals was greatly impaired. Their ability to send signals was not affected — other sodium channels inside the cell enable neuronal firing.
Eliminating Nav1.7 in specific weight-regulating neurons in mice impacted the animals’ weight. Even though they were fed the same diet, mice whose AGRP neurons lacked Nav1.7 were about 10 percent lighter than normal mice, whereas mice that lacked Nav1.7 in appetite-suppressing POMC neurons were about 10 percent heavier. Strikingly, loss of Nav1.7 in a third population called PVH neurons caused mice to nearly double their body weight in one month. Since neurons without the Nav1.7 channel were still able to to send signals, the scientists attributed the body weight changes to the cells’ inability to integrate incoming information.
Further research is needed to determine whether the Nav1.7 channel has the same effects on body weight in humans. If it does, Sternson says, it will be important for researchers to keep this role in mind as they explore the possibility of blocking Nav1.7 for pain relief. Researchers developing potential pain therapeutics might want to avoid blocking Nav1.7 channels in the brain, targeting instead channels in sensory neurons throughout the body, he says. Targeting specific Nav1.7 channels in the brain might have a benefit, however. Sternson says reducing hunger-mediating neurons’ ability to integrate incoming information might be one way to aid weight loss.
Source: Howard Hughes Medical Institute’s Janelia Research Campus
Categories: Breaking News, Leadership in Health, Leadership in Medicine
















